Salinity intrusion in coastal Bangladesh presented critical challenges to both health and livelihoods, particularly in communities reliant on saline-exposed water sources and occupations. This study investigated how environmental salinity exposure and related socio-demographic and resilience factors influenced dermatological health outcomes in coastal Bangladesh. A cross-sectional survey of 400 randomly selected households was conducted in Gabura Union, Shyamnagar subdistrict, complemented by seven focus group discussions (FGDs) to triangulate findings. Probit regression analysis revealed that using unsafe drinking water (45.2%, p < 0.001), living more than 1 km from a safe source (17.1%, p < 0.001), and working in salinity-linked occupations (14.3%, p < 0.001) significantly increased the likelihood of reporting skin disease. Notably, higher coping capacity was also associated with an increased probability of skin disease (2.3%, p< 0.05), which appeared counterintuitive. While gender was significant in the bivariate analysis, it did not remain significant in the multivariate model. However, FGDs and KIIs supported the overall findings, highlighting occupational exposure, water insecurity, and gendered vulnerabilities as key contributors to dermatological health risks. Although the study revealed important associations, its cross-sectional design and reliance on self-reported symptoms limited causal inference and biochemical specificity. The findings underscore the urgent need for comprehensive policy measures that advance sustainable water resource management, promote alternative livelihood strategies, and strengthen access to dermatological healthcare in coastal communities.
- Open Access
- Article
Salinity and Livelihoods: Dermatological Health Challenges in Coastal Bangladesh
- Md. Mahfuz Hossain 1,2,
- Indrajit Pal 1,
- Md. Anwarul Abedin 3,*,
- Sanjida Hossain Setu 4,
- Md. Shamsuzzoha 4
Author Information
Received: 11 Dec 2025 | Revised: 02 Mar 2026 | Accepted: 09 Mar 2026 | Published: 16 Apr 2026
Abstract
Graphical Abstract
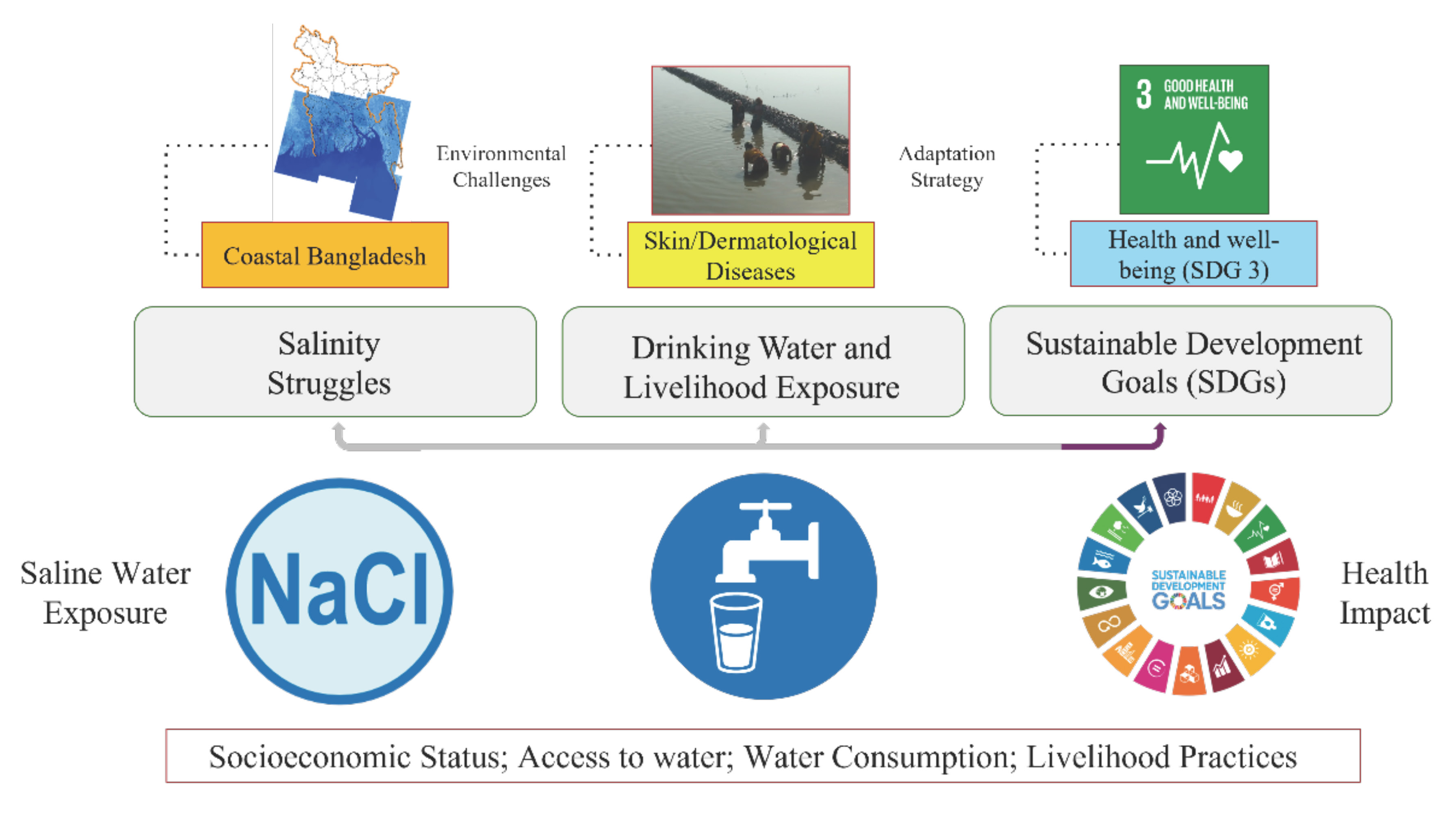
Keywords
salinity | dermatological/skin disease | health impact | livelihoods | coastal bangladesh
References
- 1.
Bhowmick, B.; Uddin, Z.; Rahman, S. Salinity Changes in South West Bangladesh and Its Impact on Rural Livelihoods. Bangladesh J. Vet. Med. 2017, 14, 251–255. https://doi.org/10.3329/bjvm.v14i2.31405.
- 2.
Islam, Md. A. Impact of Salinity Intrusion on Coastal Agriculture and Farmer's Livelihoods in Bangladesh. Asian J. Environ. Ecol. 2021, 16, 52–60. https://doi.org/10.9734/ajee/2021/v16i330251.
- 3.
Alam, M.; Morshed, M.; Tsusaka, T.W.; Pramanik, M. Awareness of impacts of salinity intrusion on livelihoods: Evidence from southern coastal rural areas of Bangladesh. Curr. Res. Environ. Sustain. 2025, 9, 100293. https://doi.org/10.1016/j.crsust.2025.100293.
- 4.
Shapna, K.J.; Li, J.; Kabir, M.H.; et al. Strengthening adaptation in coastal Bangladesh: Community-based approaches for sustainable agriculture and water management. Disaster Prev. Resil. 2024, 3, 5. https://doi.org/10.20517/dpr.2023.41.
- 5.
Akter, T.; Al, M.; Hoque, A.; et al. Coastal Flood Induced Salinity Intrusion Risk Assessment Using a Spatial Multi-criteria Approach in the South-Western Bangladesh. Earth Syst. Environ. 2025, 9, 31–49. https://doi.org/10.1007/s41748-024-00399-9.
- 6.
Morshed, M.; Tsusaka, T.W.; Pramanik, M. Impacts of salinity intrusion on livelihood assets: Evidence from the southern regions of Bangladesh. Environ. Sustain. Indic. 2026, 29, 101113.
- 7.
Akhter, T.; Naz, M.; Salehin, M.; et al. Hydrogeologic Constraints for Drinking Water Security in Southwest Coastal Bangladesh: Implications for Sustainable Development Goal 6.1. Water 2023, 15, 2333. https://doi.org/10.3390/w15132333.
- 8.
Bain, R.; Johnston, R.; Slaymaker, T. Drinking water quality and the SDGs. npj Clean Water 2020, 3, 7–9. https://doi.org/10.1038/s41545-020-00085-z.
- 9.
Biswas, S.; Adhikary, M.; Alam, A.; Roy, R. Disparities in access to water, sanitation, and hygiene (WASH) services and the status of SDG-6 implementation across districts and states in India. Heliyon 2024, 10, e37646. https://doi.org/10.1016/j.heliyon.2024.e37646.
- 10.
Hossain, M.; Pal, I.; Ahmad, M.M.; Loc, H.H. Conceptualizing Saline Exposure Model (SEM) for Health Impacts in the Delta Community in Bangladesh: A Systematic Literature Review and Field Observations. Environ. Claims J. 2025. https://doi.org/10.1080/10406026.2025.2504508.
- 11.
Agoubi, B. A review: Saltwater intrusion in North Africa's coastal areas—Current state and future challenges. Environ. Sci. Pollut. Res. 2021, 28, 17029–17043. https://doi.org/10.1007/s11356-021-12741-z.
- 12.
Negacz, K.; Malek, Ž.; de Vos, A.; Vellinga, P. Saline soils worldwide: Identifying the most promising areas for saline agriculture. J. Arid Environ. 2022, 203, 104775. https://doi.org/10.1016/j.jaridenv.2022.104775.
- 13.
Rahaman, M.A.; Rahman, M.M.; Nazimuzzaman, M. Impact of Salinity on Infectious Disease Outbreaks: Experiences from the Global Coastal Region. In Handbook of Climate Change Resilience; Springer, 2020; pp 415–424. https://doi.org/10.1007/978-3-319-95681-7_106.
- 14.
Ashrafuzzaman, M.; Artemi, C.; Santos, F.D.; Schmidt, L. Current and Future Salinity Intrusion in the South-Western Coastal Region of Bangladesh. Span. J. Soil Sci. 2022, 12, 10017. https://doi.org/10.3389/sjss.2022.10017.
- 15.
Ahmad, H. Coastal Zone Management Bangladesh Coastal Zone Management Status and Future Trends. J. Coast. Zone Manag. 2019, 22, 466.
- 16.
SRDI. Saline Soils of Bangladesh; Soil Resource Development Institute, SRMAF Project, Ministry of Agriculture: Dhaka, Bangladesh, 2010.
- 17.
Minar, M.H.; Hossain, M.B.; Shamsuddin, M.D. Climate Change and Coastal Zone of Bangladesh: Vulnerability, Resilience and Adaptability. Middle East J. Sci. Res. 2013, 13, 114–120. https://doi.org/10.5829/idosi.mejsr.2013.13.1.64121.
- 18.
Shammi, M.; Rahman, M.M.; Bondad, S.E.; Bodrud-Doza, M. Impacts of salinity intrusion in community health: A review of experiences on drinking water sodium from coastal areas of Bangladesh. Healthcare 2019, 7, 50. https://doi.org/10.3390/healthcare7010050.
- 19.
Asma, K.M.; Kotani, K. Salinity and Water-Related Disease Risk in Coastal Bangladesh. EcoHealth 2021, 18, 61–75. https://doi.org/10.1007/s10393-021-01517-z.
- 20.
Hossain, M.M.; Pal, I. Reproductive health challenges in coastal Bangladesh: A silent threat of water salinity. BMC Women's Health 2025, 25, 466. https://doi.org/10.1186/s12905-025-03989-5.
- 21.
Mahmuduzzaman, M.; Ahmed, U.; Nuruzzaman, A.K.M.; et al. Causes of Salinity Intrusion in Coastal Belt of Bangladesh. Int. J. Plant Res. 2014, 4, 8–13. https://doi.org/10.5923/s.plant.201401.02.
- 22.
Akib Jabed, M.; Paul, A.; Nath, T.K. Peoples' Perception of the Water Salinity Impacts on Human Health: A Case Study in South-Eastern Coastal Region of Bangladesh. Expo. Health 2020, 12, 41–50. https://doi.org/10.1007/s12403-018-0283-0.
- 23.
Chakraborty, R.; Khan, K.M.; Dibaba, D.T.; et al. Health implications of drinking water salinity in coastal areas of Bangladesh. Int. J. Environ. Res. Public Health 2019, 16, 3746. https://doi.org/10.3390/ijerph16193746.
- 24.
Islam, P.; Khatun, P.; Islam, A. Salinity: A chain to be assessed. J. Biosci. Agric. Res. 2022, 29, 2416–2425. https://doi.org/10.18801/jbar.290122.293.
- 25.
Vineis, P.; Chan, Q.; Khan, A. Climate change impacts on water salinity and health. J. Epidemiol. Glob. Health 2011, 1, 5–10. https://doi.org/10.1016/j.jegh.2011.09.001.
- 26.
Khan, A.E.; Ireson, A.; Kovats, S.; et al. Drinking water salinity and maternal health in coastal Bangladesh: Implications of climate change. Environ. Health Perspect. 2011, 119, 1328–1332. https://doi.org/10.1289/ehp.1002804.
- 27.
Palaniselvan, G.; Govindhan, P.; Jayganesh, D.; Kumar, M.D. Water quality assessment: A case study in the Tuticorin district of Tamil Nadu in South India. Urban Water J. 2024, 21, 565–577. https://doi.org/10.1080/1573062X.2024.2312525.
- 28.
Abedin, M.A.; Habiba, U.; Shaw, R. Community Perception and Adaptation to Safe Drinking Water Scarcity: Salinity, Arsenic, and Drought Risks in Coastal Bangladesh. Int. J. Disaster Risk Sci. 2014, 5, 110–124. https://doi.org/10.1007/s13753-014-0021-6.
- 29.
Paul, A.; Jabed, M.A. Salinity Has Made Our Life Terrible: A Qualitative Investigation of Human Sufferings in the Chittagong Coast. Orient. Geogr. 2018, 59, 1–18.
- 30.
Yakupu, A.; Aimaier, R.; Yuan, B.; et al. The burden of skin and subcutaneous diseases: Findings from the global burden of disease study 2019. Front. Public Health 2023, 11, 1145513. https://doi.org/10.3389/fpubh.2023.1145513.
- 31.
Chen, W.; Mempel, M.; Traidl-Hofmann, C.; et al. Gender aspects in skin diseases. J. Eur. Acad. Dermatol. Venereol. 2010, 24, 1378–1385. https://doi.org/10.1111/j.1468-3083.2010.03668.x.
- 32.
Desai, M.K.; Brinton, R.D. Autoimmune disease in women: Endocrine transition and risk across the lifespan. Front. Endocrinol. 2019, 10, 265. https://doi.org/10.3389/fendo.2019.00265.
- 33.
Lagacé, F.; D’Aguanno, K.; Prosty, C.; et al. The Role of Sex and Gender in Dermatology—From Pathogenesis to Clinical Implications. J. Cutan. Med. Surg. 2023, 27, NP1–NP36. https://doi.org/10.1177/12034754231177582.
- 34.
Zhang, H.; Wang, M.; Zhao, X.; et al. Role of stress in skin diseases: A neuroendocrine-immune interaction view. Brain Behav. Immun. 2024, 116, 286–302. https://doi.org/10.1016/j.bbi.2023.12.005.
- 35.
Richard, M.A.; Paul, C.; Nijsten, T.; et al. Prevalence of most common skin diseases in Europe: A population-based study. J. Eur. Acad. Dermatol. Venereol. 2022, 36, 1088–1096. https://doi.org/10.1111/jdv.18050.
- 36.
Parker, E.R.; Mo, J.; Goodman, R.S. The dermatological manifestations of extreme weather events: A comprehensive review of skin disease and vulnerability. J. Clim. Change Health 2022, 8, 100162. https://doi.org/10.1016/j.joclim.2022.100162.
- 37.
Soni, K. Study of Various Skin Disorders in Children in Health Training Centres of Etawah District, Uttar Pradesh: A Cross-Sectional Study. Int. J. Healthc. Educ. Med. Inform. 2022, 9, 20–23. https://doi.org/10.24321/2455.9199.202204.
- 38.
Raghupathi, V.; Raghupathi, W. The Influence of Education on Health: An empirical assessment of OECD countries for the period 1995–2015. Arch. Public Health 2020, 78, 20.
- 39.
Meherali, S.; Punjani, N.S.; Mevawala, A. Health Literacy Interventions to Improve Health Outcomes in Low- and Middle-Income Countries. Health Lit. Res. Pract. 2020, 4, e251–e266. https://doi.org/10.3928/24748307-20201118-01.
- 40.
Roy, B.; Penha-Lopes, G.P.; Uddin, M.S.; et al. Sea level rise induced impacts on coastal areas of Bangladesh and local-led community-based adaptation. Int. J. Disaster Risk Reduct. 2022, 73, 102905. https://doi.org/10.1016/j.ijdrr.2022.102905.
- 41.
Ashrafuzzaman, M.; Gomes, C.; Guerra, J. The Changing Climate Is Changing Safe Drinking Water, Impacting Health: A Case in the Southwestern Coastal Region of Bangladesh (SWCRB). Climate 2023, 11, 146. https://doi.org/10.3390/cli11070146.
- 42.
Al Nahian, M.; Ahmed, A.; Lázár, A.N.; et al. Drinking water salinity associated health crisis in coastal Bangladesh. Elementa 2018, 6, 2. https://doi.org/10.1525/elementa.143.
- 43.
Nauges, C.; Strand, J. Water Hauling and Girls’ School Attendance: Some New Evidence from Ghana. Environ. Resour. Econ. 2017, 66, 65–88. https://doi.org/10.1007/s10640-015-9938-5.
- 44.
Begum, M.; Morshed, M.S.; Islam, R.; Nisa, M.M.I. Household Water, Sanitation, Hygiene Facilities and Practices in Selected Villages of Taraganj Upazilla, Rangpur. J. Rangpur Med. Coll. 2023, 8, 53–58. https://doi.org/10.3329/jrpmc.v8i1.65060.
- 45.
Sachdev, R.; Mathur, M.L.; Haldiya, K.R.; Saiyed, H.N. Work-related health problems in salt workers of Rajasthan, India. Indian J. Occup. Environ. Med. 2006, 10, 62–64.
- 46.
Anderson, S.E.; Meade, B.J. Occupational Immunotoxicology. In Comprehensive Toxicology, 3rd ed.; Elsevier, 2018. https://doi.org/10.1016/B978-0-12-801238-3.64239-3.
- 47.
Harel, N.; Reshef, L.; Biran, D.; et al. Skin microbiome of people living at the Dead Sea area—The lowest place on earth. Res. Microbiol. 2023, 174, 104059. https://doi.org/10.1016/j.resmic.2023.104059.
- 48.
Manoharan, P.; Kaliaperumal, K. Salt and skin. Int. J. Dermatol. 2022, 61, 291–298. https://doi.org/10.1111/ijd.15588.
- 49.
Cherian, J.; Singh, Z.; Bazroy, J.; et al. Study of morbidity pattern among salt workers in Marakkanam, Tamil Nadu, India. J. Clin. Diagn. Res. 2015, 9, LC01–LC03. https://doi.org/10.7860/JCDR/2015/13651.5827.
- 50.
Vasudevan, J.; Vaithiyalingam, S.; Anandan, V.; et al. Common morbidities and felt needs of salt pan workers in a coastal area of Tamil Nadu, India. Int. J. Res. Med. Sci. 2019, 7, 805. https://doi.org/10.18203/2320-6012.ijrms20190927.
- 51.
Schafer, P.; Bewick-Sonnatag, C.; Capri, M.G.; Berardesca, E. Physiological Changes in Skin Barrier Function in Relation to Occlusion Level. Ski. Pharmacol. Appl. Ski. Physiol. 2002, 15, 7–19.
- 52.
Firooz, A.; Aghazadeh, N.; Rajabi Estarabadi, A.; Hejazi, P. The effects of water exposure on biophysical properties of normal skin. Ski. Res. Technol. 2015, 21, 131–136. https://doi.org/10.1111/srt.12167.
- 53.
Fartasch, M.; Taeger, D.; Broding, H.C.; et al. Evidence of increased skin irritation after wet work: Impact of water exposure and occlusion. Contact Dermat. 2012, 67, 217–228. https://doi.org/10.1111/j.1600-0536.2012.02063.x.
- 54.
Pathmanaban, O.N.; Porter, J.S.; White, I.R. Dogger Bank itch in the eastern English Channel: A newly described geographical distribution of an old problem. Clin. Exp. Dermatol. 2005, 30, 622–626. https://doi.org/10.1111/j.1365-2230.2005.01932.x.
- 55.
Tolon, M.T.; Karacalar, U.; Şirin, C. Observation of Vibrio mediterranei (Pujalte and Garay 1986) / Vibrio shiloi (Kushmaro et al. 2001) bacteria from skin ulcers of the cultured sea cucumber Holothuria poli (Delle Chiaje, 1823). Ege J. Fish. Aquat. Sci. 2021, 38, 393–397. https://doi.org/10.12714/egejfas.38.3.16.
- 56.
Krajina, I.; Stupin, A.; Šola, M.; Mihalj, M. Oxidative Stress Induced by High Salt Diet—Possible Implications for Development and Clinical Manifestation of Cutaneous Inflammation and Endothelial Dysfunction in Psoriasis vulgaris. Antioxidants 2022, 11, 1269. https://doi.org/10.3390/antiox11071269.
- 57.
Few, R.; Scott, Z.; Wooster, K.; et al. Strengthening capacities for disaster risk management II: Lessons for effective support. Int. J. Disaster Risk Reduct. 2016, 20, 154–162. https://doi.org/10.1016/j.ijdrr.2016.02.005.
- 58.
Al-Ruzzieh, M.A.; Ayaad, O. Work Stress, Coping Strategies, and Health-Related Quality of Life Among Nurses at an International Specialized Cancer Center. Asian Pac. J. Cancer Prev. 2021, 22, 2995–3004. https://doi.org/10.31557/APJCP.2021.22.9.2995.
- 59.
Kugbey, N.; Meyer-Weitz, A.; Oppong Asante, K. Mental adjustment to cancer and quality of life among women living with breast cancer in Ghana. Int. J. Psychiatry Med. 2019, 54, 217–230. https://doi.org/10.1177/0091217418805087.

This work is licensed under a Creative Commons Attribution 4.0 International License.


