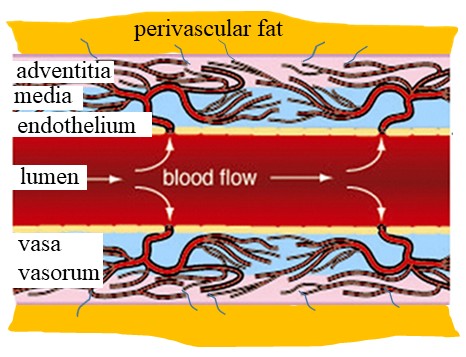
The vasa vasorum, a network of microvessels providing the vessel wall with oxygen and nutrients, is more dense and penetrates deeper in veins than in arteries. The saphenous vein is the most commonly used conduit for coronary artery bypass surgery but its patency is inferior to the ‘gold standard’ internal thoracic artery. Considerable vascular damage is caused during conventional preparation of the saphenous vein that effects all vessel layers, the endothelium and intima, the media and the adventitia. Graft patency is dramatically improved when the vein is harvested intact and with minimal trauma using the no touch technique. Among the structures preserved is the vasa vasorum that is suggested to play a role in the superior patency rate of no touch saphenous vein grafts. Histological studies have identified regions of the saphenous vein that are proposed to represent termination of vasa vasorum in the lumen. Since the vasa vasorum of the explanted saphenous vein graft is disconnected from its arterial blood supply in vivo an inside out/outside in communication has been hypothesised based on ex vivo perfusion studies. Such a novel transport system may play an important role in maintaining blood supply to the vessel wall, extending to the outermost capillary network of the perivascular fat. Also, bidirectional transport of vasoprotective factors such as nitric oxide may contribute to the underlying mechanisms involved in the improved performance of no touch saphenous vein grafts.
- Open Access
- Review
What Is the Fate of Saphenous Vein Graft Vasa Vasorum after Coronary Artery Bypass Surgery: An Open-and-Shut Case?
Author Information
Received: 20 Dec 2025 | Revised: 16 Jan 2026 | Accepted: 25 Feb 2026 | Published: 18 Mar 2026
Abstract
Graphical Abstract
Keywords
saphenous vein | vasa vasorum | CABG | blood flow | patency
References
- 1.
World Health Organization. Cardiovascular Diseases (CVDs). Available online: http://www.who.int/mediacentre/factsheets/fs317/en/ (accessed on 22 December 2025).
- 2.
Dimeling, G.; Bakaeen, L.; Khatri, J.; et al. CABG: When, why, and how? Clevel. Clin. J. Med. 2021, 88, 295–303.
- 3.
Tsui, J.C.; Dashwood, M.R. Recent strategies to reduce vein graft occlusion: A need to limit the effect of vascular damage. Eur. J. Vasc. Endovasc. Surg. 2002, 23, 202–208. https://doi.org/10.1053/ejvs.2002.1600.
- 4.
Alzghari, T.; Dimagli, A.; An, K.R.; et al. Conduits and Strategies for Arterial Revascularization in CABG. Rev. Cardiovasc. Med. 2023, 24, 188. https://doi.org/10.31083/j.rcm2407188.
- 5.
Gaudino, M.F.L.; Spadaccio, C.; Taggart, D.P. State-of-the-Art Coronary Artery Bypass Grafting: Patient Selection, Graft Selection, and Optimizing Outcomes. Interv. Cardiol. Clin. 2019, 8, 173–198. https://doi.org/10.1016/j.iccl.2018.11.007.
- 6.
Taggart, D.P. Current status of arterial grafts for coronary artery bypass grafting. Ann. Cardiothorac. Surg. 2013, 2, 427–430. https://doi.org/10.3978/j.issn.2225-319X.2013.07.21.
- 7.
Schwann, T.A.; Tatoulis, J.; Puskas, J.; et al. Worldwide Trends in Multi-arterial Coronary Artery Bypass Grafting Surgery 2004–2014: A Tale of 2 Continents. Semin. Thorac. Cardiovasc. Surg. 2017, 29, 273–280. https://doi.org/10.1053/j.semtcvs.2017.05.018.
- 8.
Audisio, K.; Halbreiner, M.S.; Chadow, D.; et al. Radial artery or saphenous vein for coronary artery bypass grafting. Trends Cardiovasc. Med. 2022, 32, 479–484. https://doi.org/10.1016/j.tcm.2021.09.007.
- 9.
Souza, D. A new no-touch preparation technique: Technical notes. Scand. J. Thorac. Cardiovasc. Surg. 1996, 30, 41–44. https://doi.org/10.3109/14017439609107239.
- 10.
Souza, D.S.; Arbeus, M.; Botelho Pinheiro, B.; et al. The no-touch technique of harvesting the saphenous vein for coronary artery bypass grafting surgery. Multimed Man Cardiothorac Surg. 2009, 2009, mmcts-2008.
- 11.
Dreifaldt, M.; Souza, D.S.; Loesch, A.; et al. The “no-touch” harvesting technique for vein grafts in coronary artery bypass surgery preserves an intact vasa vasorum. J. Thorac. Cardiovasc. Surg. 2011, 141, 145–150. https://doi.org/10.1016/j.jtcvs.2010.02.005.
- 12.
Johansson, B.L.; Souza, D.S.; Bodin, L.; et al. No touch vein harvesting technique for CABG improves the long-term clinical outcome. Scand. Cardiovasc. J. 2009, 43, 63–68. https://doi.org/10.1080/14017430802140104.
- 13.
Samano, N.; Geijer, H.; Liden, M.; et al. The no-touch saphenous vein for coronary artery bypass grafting maintains a patency, after 16 years, comparable to the left internal thoracic artery: A randomized trial. J. Thorac. Cardiovasc. Surg. 2015, 150, 880–888. https://doi.org/10.1016/j.jtcvs.2015.07.027.
- 14.
Souza, D.S.; Bomfim, V.; Skoglund, H.; et al. High early patency of saphenous vein graft for coronary artery bypass harvested with surrounding tissue. Ann. Thorac. Surg. 2001, 71, 797–800. https://doi.org/10.1016/s0003-4975(00)02508-x.
- 15.
Dreifaldt, M.; Mannion, J.D.; Geijer, H.; et al. The no-touch saphenous vein is an excellent alternative conduit to the radial artery 8 years after coronary artery bypass grafting: A randomized trial. J. Thorac. Cardiovasc. Surg. 2021, 161, 624–630. https://doi.org/10.1016/j.jtcvs.2019.09.177.
- 16.
Dashwood, M.R.; Loesch, A. Arterial versus venous conduits in coronary artery bypass surgery: Comparing apples with oranges. J. Thorac. Cardiovasc. Surg. 2019, 157, e253–e254. https://doi.org/10.1016/j.jtcvs.2018.11.047.
- 17.
Gaudino, M.; Benedetto, U.; Fremes, S.; et al. Radial-Artery or Saphenous-Vein Grafts in Coronary-Artery Bypass Surgery. N. Engl. J. Med. 2018, 378, 20.
- 18.
Kopjar, T.; Dashwood, M.R.; Dreifaldt, M.; et al. No-touch saphenous vein as an important conduit of choice in coronary bypass surgery. J. Thorac. Dis. 2018, 10, S3292–S3296. https://doi.org/10.21037/jtd.2018.08.
- 19.
Dell’Aquila, M.; Prapas, S.; Falco, G.; et al. Saphenous Vein Graft and Nitric Oxide: Strategies to Prevent Graft Failure and Enhance Patency in Coronary Artery Bypass Grafting. Front. Cardiovasc. Med. 2026, 12, 1745260. https://doi.org/10.3389/fcvm.2025.1745260.
- 20.
Sandner, S.; Hirofuji, A.; Mantaj, P.; et al. Outcomes of No-Touch Vs Conventionally Harvested Saphenous Veins for Coronary Artery Bypass Surgery: A Meta-Analysis of Randomized Trials. Eur. J. Cardio-Thorac. Surg. 2025, 67, ezaf297. https://doi.org/10.1093/ejcts/ezaf297.
- 21.
Ali, M.A.; Alam, U.; Khattak, F.; et al. Comparative efficacy and safety of no-touch versus conventional vein harvesting techniques in coronary artery bypass grafting: A systematic review and meta-analysis. Open Heart 2025, 12, e003391. https://doi.org/10.1136/openhrt-2025-003391.
- 22.
Chen, X.J.; Zhang, J.; Li, W.D.; et al. Interpretation on Expert systematic review on the choice of conduits for coronary artery bypass grafting endorsed by the European Association for Cardio-Thoracic Surgery and the Society of Thoracic Surgeons in 2023. Chin. J. Surg. 2023, 62, 45–49. https://doi.org/10.3760/cma.j.cn112139-20230917-00126.
- 23.
Gaudino, M.; Hameed, I.; Robinson, N.B.; et al. Angiographic Patency of Coronary Artery Bypass Conduits: A Network Meta-Analysis of Randomized Trials. J. Am. Heart Assoc. 2021, 10, e019206. https://doi.org/10.1161/JAHA.120.019206.
- 24.
Liu, C.; Zhang, M.X.; Guan, X.L.; et al. Techniques for harvesting the saphenous vein in coronary artery bypass grafting: A network systematic review and meta-analysis. Open Heart 2025, 12, e003728. https://doi.org/10.1136/openhrt-2025-003728.
- 25.
Yokoyama, Y.; Takagi, H.; Kuno, T. Graft Patency of a Second Conduit for Coronary Artery Bypass Surgery: A Network Meta-Analysis of Randomized Controlled Trials. Semin. Thorac. Cardiovasc. Surg. 2022, 34, 102–109. https://doi.org/10.1053/j.semtcvs.2021.02.002.
- 26.
Lumsden, A.B.; Eaves, F.F.; Ofenloch, J.C.; et al. Subcutaneous, video-assisted saphenous vein harvest: Report of the first 30 cases. Cardiovasc. Surg. 1996, 4, 771–776.
- 27.
Dacey, L.J.; Braxton, J.H.; Kramer, R.S.; et al. Long-term outcomes of endoscopic vein harvesting after coronary artery bypass grafting. Circulation 2011, 123, 147–153.
- 28.
Kopjar, T.; Dashwood, M.R. Endoscopic Versus “No-Touch” Saphenous Vein Harvesting for Coronary Artery Bypass Grafting: A Trade-Off between Wound Healing and Graft Patency. Angiology 2016, 67, 121–132. https://doi.org/10.1177/0003319715584126.
- 29.
Kopjar, T.; Dashwood, M.R. Towards Endoscopic No-Touch Saphenous Vein Graft Harvesting in Coronary Bypass Surgery. Braz. J. Cardiovasc. Surg. 2022, 37, 57–65. https://doi.org/10.21470/1678-9741-2022-0144.
- 30.
Kiani, S.; Poston, R. Is endoscopic harvesting bad for saphenous vein graft patency in coronary surgery? Curr. Opin. Cardiol. 2011, 26, 518–522.
- 31.
Nowicki, M.; Buczkowski, P.; Miskowiak, B.; et al. Immunocytochemical study on endothelial integrity of saphenous vein grafts harvested by minimally invasive surgery with the use of vascular mayo stripers. A randomized controlled trial. Eur. J. Vasc. Endovasc. Surg. 2004, 27, 244–250.
- 32.
Kopjar, T.; Ivankovic, S.; Lima, M.L.; et al. Endoscopic or No-Touch Vein Harvesting for CABG: What is Best for the Patient? Braz. J. Cardiovasc. Surg. 2016, 31, 461–464. https://doi.org/10.5935/1678-9741.20160091.
- 33.
Hayashi, I.; Kashima, I.; Yoshikawa, E. Use of the No-Touch Saphenous Vein Harvesting Technique via Small Incisions. Innovations 2020, 15, 81–84. https://doi.org/10.1177/1556984519886549.
- 34.
Katayama, Y.; Miho, T.; Nogami, E.; et al. Endoscopic Pedicle Saphenous Vein Graft Harvesting. Ann. Thorac. Cardiovasc. Surg. 2024, 30, 23–00054. https://doi.org/10.5761/atcs.nm.23-00054.
- 35.
Yoshino, K.; Abe, K.; Suzuki, K.; et al. A Novel Technique of Endoscopic Vein Harvesting with Preserved Perivascular Tissue. Innovations 2020, 15, 475–477. https://doi.org/10.1177/1556984520948139.
- 36.
Yoshino, K.; Kikuchi, K.; Tamaki, R.; et al. A Novel Technique of No-Touch Endoscopic Saphenous Vein Harvesting. Innovations 2023, 18, 589–591. https://doi.org/10.1177/15569845231210299.
- 37.
Kim, J.; Sohn, S.H.; Choi, J.S.; et al. Graft Patency of No-Touch Saphenous Veins Used as Aortocoronary Bypass Grafts. J. Chest Surg. 2023, 56, 313–321. https://doi.org/10.5090/jcs.23.027.
- 38.
Milutinović, A.; Klajević, J.; Živković, I.; et al. Early Experiences of Serbian Surgeons Using No-Touch Technique for Vein Conduits in CABG Patients: A Follow-Up Study with Multi-Slice CT Angiography. Medicina 2024, 60, 1427. https://doi.org/10.3390/medicina60091427.
- 39.
Tian, M.; Wang, X.; Sun, H.; et al. No-Touch Versus Conventional Vein Harvesting Techniques at 12 Months After Coronary Artery Bypass Grafting Surgery: Multicenter Randomized, Controlled Trial. Circulation 2021, 144, 1120–1129. https://doi.org/10.1161/CIRCULATIONAHA.121.055525.
- 40.
Tian, M.; Wang, X.; Feng, W.; et al. No-touch versus conventional vein in coronary artery bypass grafting: Three year follow-up of multicentre randomised PATENCY trial. BMJ 2025, 389, e082883. https://doi.org/10.1136/bmj-2024-082883.
- 41.
Angelini, G.D.; Johnson, T.; Culliford, L.; et al. Comparison of alternate preparative techniques on wall thickness in coronary artery bypass grafts: The HArVeST randomized controlled trial. J. Card. Surg. 2021, 36, 1985–1995. https://doi.org/10.1111/jocs.15477.
- 42.
Deb, S.; Singh, S.K.; de Souza, D.; et al. SUPERIOR SVG: No touch saphenous harvesting to improve patency following coronary bypass grafting (a multi-centre randomized control trial, NCT01047449). J. Cardiothorac. Surg. 2019, 14, 85. https://doi.org/10.1186/s13019-019-0887-x.
- 43.
Ragnarsson, S.; Janiec, M.; Modrau, I.S.; et al. No-touch saphenous vein grafts in coronary artery surgery (SWEDEGRAFT): Rationale and design of a multicenter, prospective, registry-based randomized clinical trial. Am. Heart J. 2020, 224, 17–24. https://doi.org/10.1016/j.ahj.2020.03.009.
- 44.
Thelin, S.; Modrau, I.S.; Duvernoy, O.; et al. No-touch vein grafts in coronary artery bypass surgery: A registry-based randomized clinical trial. Eur. Heart J. 2025, 46, 1720–1729. https://doi.org/10.1093/eurheartj/ehaf018.
- 45.
Weiss, M.G.; Nielsen, P.H.; James, S.; et al. Clinical Outcomes After Surgical Revascularization Using No-Touch Versus Conventional Saphenous Vein Grafts: Mid-Term Follow-Up of Propensity Score Matched Cohorts. Semin. Thorac. Cardiovasc. Surg. 2023, 35, 228–236. https://doi.org/10.1053/j.semtcvs.2021.12.002.
- 46.
Gaudino, M.; Sandner, S. The SWEDEGRAFT trial: When absence of evidence is not evidence of absence. Eur. Heart J. 2025, 46, 1730–1732. https://doi.org/10.1093/eurheartj/ehaf043.
- 47.
Dashwood, M.R.; Celik, Z.; Topal, G. Reducing vasospasm of vein and arterial conduits used in coronary artery bypass surgery: Are solutions the solution or is preserved perivascular fat the answer? Front. Physiol. 2025, 16, 1539102. https://doi.org/10.3389/fphys.2025.1539102.
- 48.
He, G.-W.; Taggart, D.P. Spasm in Arterial Grafts in Coronary Artery Bypass Grafting Surgery. Ann. Thorac. Surg. 2016, 101, 1222–1229. https://doi.org/10.1016/j.athoracsur.2015.09.071.
- 49.
Zheng, D.; Zhang, L.; Yang, M.D.; et al. Use of Radial Artery Grafts for Coronary Artery Bypass Grafting. Heart Surg. Forum 2022, 25, E385–E390. https://doi.org/10.1532/hsf.4697.
- 50.
Rueda, F.; Souza, D.; Lima, R.D.C.; et al. Novel no-touch technique of harvesting the saphenous vein for coronary artery bypass grafting. Arq. Bras. Cardiol. 2008, 90, 356–362. https://doi.org/10.1590/s0066-782x2008000600002.
- 51.
Favaloro, R.G. Saphenous vein autograft replacement of severe segmental coronary artery occlusion: Operative technique. Ann. Thorac. Surg. 1968, 5, 334–339. https://doi.org/10.1016/s0003-4975(10)66351-5.
- 52.
Favaloro, R.G. Saphenous vein graft in the surgical treatment of coronary artery disease. Operative technique. J. Thorac. Cardiovasc. Surg. 1969, 58, 178–185.
- 53.
Dashwood, M.R. No-Touch Saphenous Vein—Vascular Damage and the London Connection. Braz. J. Cardiovasc. Surg. 2022, 37, 1–6. https://doi.org/10.21470/1678-9741-2022-0024.
- 54.
Gomes, W.J.; Kim, K.B.; Pinheiro, B.B.; et al. The No-touch Saphenous Vein Graft in Coronary Artery Bypass Surgery. Towards a New Standard? Braz. J. Cardiovasc. Surg. 2022, 37, I–II. https://doi.org/10.21470/1678-9741-2022-0955.
- 55.
Pinheiro, B.B.; Dashwood, M.; Souza, D.S.R. The “No-touch” Harvesting Technique Revives the Position of the Saphenous Vein as an Important Conduit in CABG Surgery: 30-year Anniversary. Braz. J. Cardiovasc. Surg. 2021, 36, I–III. https://doi.org/10.21470/1678-9741-2021-0959.
- 56.
Souza, D.S.; Johansson, B.; Bojö, L.; et al. Harvesting the saphenous vein with surrounding tissue for CABG provides long-term graft patency comparable to the left internal thoracic artery: Results of a randomized longitudinal trial. The J. Thorac. Cardiovasc. Surg. 2006, 132, 373–378. https://doi.org/10.1016/j.jtcvs.2006.04.002.
- 57.
Dashwood, M.R.; Tsui, J.C. ‘No-touch’ saphenous vein harvesting improves graft performance in patients undergoing coronary artery bypass surgery: A journey from bedside to bench. Vasc. Pharmacol. 2013, 58, 240–250. https://doi.org/10.1016/j.vph.2012.07.008.
- 58.
Dashwood, M.R.; Dooley, A.; Xu, S.-W.; et al. Does periadventitial fat-derived nitric oxide play a role in improved saphenous vein graft patency in patients undergoing coronary artery bypass surgery? J. Vasc. Res. 2007, 44, 175–181. https://doi.org/10.1159/000099833.
- 59.
Fernandez-Alfonso, M.S.; Souza, D.S.; Dreifaldt, M.; et al. Commentary: Perivascular Fat and Improved Vein Graft Patency in Patients Undergoing Coronary Artery Bypass Surgery. Curr. Vasc. Pharmacol. 2016, 14, 308–312. https://doi.org/10.2174/1570161114666160513150444.
- 60.
Fernández-Alfonso, M.S.; Gil-Ortega, M.; Aranguez, I.; et al. Role of PVAT in coronary atherosclerosis and vein graft patency: Friend or foe? Br. J. Pharmacol. 2017, 174, 3561–3572. https://doi.org/10.1111/bph.13734.
- 61.
Dashwood, M.R.; Savage, K.; Tsui, J.C.; et al. Retaining perivascular tissue of human saphenous vein grafts protects against surgical and distension-induced damage and preserves endothelial nitric oxide synthase and nitric oxide synthase activity. J. Thorac. Cardiovasc. Surg. 2009, 138, 334–340. https://doi.org/10.1016/j.jtcvs.2008.11.060.
- 62.
Angelini, G.D.; Passani, S.L.; Breckenridge, I.M.; et al. Nature and pressure dependence of damage induced by distension of human saphenous vein coronary artery bypass grafts. Cardiovasc. Res. 1987, 21, 902–907. https://doi.org/10.1093/cvr/21.12.902.
- 63.
Roubos, N.; Rosenfeldt, F.L.; Richards, S.M.; et al. Improved preservation of saphenous vein grafts by the use of glyceryl trinitrate-verapamil solution during harvesting. Circulation 1995, 92, II31–II36. https://doi.org/10.1161/01.cir.92.9.31.
- 64.
Tsui, J.C.; Souza, D.S.; Filbey, D.; et al. Preserved endothelial integrity and nitric oxide synthase in saphenous vein grafts harvested by a ‘no-touch’ technique. Br. J. Surg. 2001, 88, 1209–1215. https://doi.org/10.1046/j.0007-1323.2001.01855.x.
- 65.
Tsui, J.C.; Souza, D.S.; Filbey, D.; et al. Localization of nitric oxide synthase in saphenous vein grafts harvested with a novel “no-touch” technique: Potential role of nitric oxide contribution to improved early graft patency rates. J. Vasc. Surgery 2002, 35, 356–362. https://doi.org/10.1067/mva.2002.121072.
- 66.
Ahmed, S.R.; Johansson, B.L.; Karlsson, M.G.; et al. Human saphenous vein and coronary bypass surgery: Ultrastructural aspects of conventional and “no-touch” vein graft preparations. Histol. Histopathol. 2004, 19, 421–433. https://doi.org/10.14670/HH-19.421.
- 67.
Saito, T.; Kurazumi, H.; Suzuki, R.; et al. Perivascular Adipose Tissue Is a Major Source of Nitric Oxide in Saphenous Vein Grafts Harvested via the No-Touch Technique. J. Am. Heart Assoc. 2022, 11, e020637. https://doi.org/10.1161/JAHA.120.020637.
- 68.
Dashwood, M.R. Keeping NO in No-Touch Saphenous Vein Bypass Grafts. Braz. J. Cardiovasc. Surg. 2026, 41, e20250040. https://doi.org/10.21470/1678-9741-2025-0040.
- 69.
Ham, A.W. Histology, 7th ed.; J. B. Lippincott & Co.: Philadelphia, PA, USA, 1974; pp. 577–581.
- 70.
Jackson, D.R. Living homologous saphenous vein. A new graft conduit for use in arterial reconstruction. Angiology 1970, 21, I–II. https://doi.org/10.1177/000331977002100101.
- 71.
Phillippi, J.A. On vasa vasorum: A history of advances in understanding the vessels of vessels. Sci. Adv. 2022, 8, eabl6364. https://doi.org/10.1126/sciadv.abl6364.
- 72.
Dreifaldt, M.; Souza, D.; Bodin, L.; et al. The vasa vasorum and associated endothelial nitric oxide synthase is more important for saphenous vein than arterial bypass grafts. Angiology 2013, 64, 293–299. https://doi.org/10.1177/0003319712443729.
- 73.
Loesch, A.; Dashwood, M. Vasa vasorum inside out/outside in communication: A potential role in the patency of saphenous vein coronary artery bypass grafts. J. Cell Commun. Signal. 2018, 12, 631–643. https://doi.org/10.1007/s12079-018-0483-1.
- 74.
Souza, D.S.; Christofferson, R.H.; Bomfim, V.; et al. “No-touch” technique using saphenous vein harvested with its surrounding tissue for coronary artery bypass grafting maintains an intact endothelium. Scand. Cardiovasc. J. 1999, 33, 323–329. https://doi.org/10.1080/14017439950141362.
- 75.
Vasilakis, V.; Dashwood, M.R.; Souza, D.S.R.; et al. Human saphenous vein and coronary bypass surgery: Scanning electron microscopy of conventional and ‘no-touch’ vein grafts. Vasc. Dis. Prev. 2004, 1, 133–139. https://doi.org/10.2174/1567270043405204.
- 76.
Dashwood, M.R.; Anand, R.; Loesch, A.; et al. Hypothesis: A potential role for the vasa vasorum in the maintenance of vein graft patency. Angiology 2004, 55, 385–395. https://doi.org/10.1177/000331970405500405.
- 77.
Barker, S.G.; Talbert, A.; Cottam, S.; et al. Arterial intimal hyperplasia after occlusion of the adventitial vasa vasorum in the pig. Arterioscler. Thromb. J. Vasc. Biol. 1993, 13, 70–77. https://doi.org/10.1161/01.atv.13.1.70.
- 78.
Barker, S.G.; Tilling, L.C.; Miller, G.C.; et al. The adventitia and atherogenesis: Removal initiates intimal proliferation in the rabbit which regresses on generation of a ‘neoadventitia’. Atherosclerosis 1994, 105, 131–144. https://doi.org/10.1016/0021-9150(94)90043-4.
- 79.
Barger, A.C.; Beeuwkes, R., 3rd; Lainey, L.L.; et al. Hypothesis: Vasa vasorum and neovascularization of human coronary arteries. A possible role in the pathophysiology of atherosclerosis. N. Engl. J. Med. 1984, 310, 175–177. https://doi.org/10.1056/NEJM198401193100307.
- 80.
Stingl, J.; Musil, V.; Pirk, J.; et al. Vasa vasorum of the failed aorto-coronary venous grafts. Surg. Radiol. Anat. 2018, 40, 769–778. https://doi.org/10.1007/s00276-018-2036-y.
- 81.
Samano, N.; Loesch, A.; Dashwood, M.R. What is the impact of preserving the endothelium on saphenous vein graft performance? Comments on the ‘NO’ touch harvesting technique. J. Cardiovasc. Surg. 2021, 16, 21. https://doi.org/10.1186/s13019-021-01397-y.
- 82.
Herbst, M.; Hölzenbein, T.J.; Minnich, B. Characterization of the Vasa Vasorum in the Human Great Saphenous Vein: A Scanning Electron Microscopy and 3D-Morphometry Study Using Vascular Corrosion Casts. Microsc. Microanal. 2014, 20, 1120–1133. https://doi.org/10.1017/S1431927614001287.
- 83.
Lametschwandtner, A.; Minnich, B.; Kachlik, D.; et al. Three-dimensional arrangement of the vasa vasorum in explanted segments of the aged human great saphenous vein: Scanning electron microscopy and three-dimensional morphometry of vascular corrosion casts. Anat. Rec. Part A Discov. Mol. Cell. Evol. Biol. 2004, 281, 1372–1382. https://doi.org/10.1002/ar.a.20098.
- 84.
Kachlik, D.; Baca, V.; Stingl, J.; et al. Architectonic arrangement of the vasa vasorum of the human great saphenous vein. J. Vasc. Res. 2007, 44, 157–166. https://doi.org/10.1159/000099142.
- 85.
Kachlík, D.; Lametschwandtner, A.; Rejmontová, J.; et al. Vasa vasorum of the human great saphenous vein. Surg. Radiol. Anat. 2003, 24, 377–381. https://doi.org/10.1007/s00276-002-0067-9.
- 86.
Brock, W.H. Vasa vasorum of veins in dogs and man. Angiology 1977, 28, 351–360. https://doi.org/10.1177/000331977702800507.
- 87.
Crotty, T.P. The role of vasa vasorum in atherosclerosis. Med. Hypotheses 1989, 28, 233–243.
- 88.
Crotty, T.P. The path of retrograde flow from thelumen of the lateral saphenous vein of the dog. Microvasc. Res. 1989, 37, 119–122.
- 89.
Ohta, O.; Kusaba, A. Development of vasa vasorum in the arterially implanted autovein bypass graft and its anastomosis in the dog. Int. Angiol. J. Int. Union Angiol. 1997, 16, 197–203.
- 90.
Loesch, A. Vasa Vasorum in Saphenous Vein for CABG: A Review of Morphological Characteristics. Braz. J. Cardiovasc. Surg. 2023, 38, e20230045. https://doi.org/10.21470/1678-9741-2023-0045.
- 91.
Loesch, A.; Dashwood, M.R. A Brief Comment on Vasa Vasorum of Human Saphenous Vein: Relevance for Coronary Artery Bypass Surgery. Braz. J. Cardiovasc. Surg. 2021, 36, 106–111. https://doi.org/10.21470/1678-9741-2020-0066.
- 92.
Loesch, A. Great Saphenous Vein Lumen: Intimal Openings. Braz. J. Cardiovasc. Surg. 2026, 41, e20240382. https://doi.org/10.21470/1678-9741-2024-0382.
- 93.
Părău, A.F.; Manzur, A.R.; Mihaicuta, S.; et al. The Controversy of Using Insufficient Great Saphenous Veins in Coronary Artery Bypass Grafting: A Comparative Morphological Analysis of Healthy and Insufficient Veins Related to the Possibility of Using Them as a Graft. Biomedicines 2024, 12, 476. https://doi.org/10.3390/biomedicines12030476.
- 94.
Bazylev, V.V.; Tungusov, D.S.; Mikulyak, A.I.; et al. Morphological assessment of autovenous conduits in the composition of perivascular adipose tissue. Angiol. Vasc. Surg. 2022, 28, 104–109. https://doi.org/10.33029/1027-6661-2022-28-1-104-109.
- 95.
Frolov, A.V.; Terekhov, A.A.; Bogdanov, L.A.; et al. Comparative study of vasa vasorum and neointima in conduits for coronary artery bypass grafting. Angiol. Vasc. Surg. 2021, 27, 121–126. https://doi.org/10.33529/ANGIO2021218.
- 96.
Nishimiya, K.; Matsumoto, Y.; Takahashi, J.; et al. Association of adventitial vasa vasorum and inflammation with coronary hyperconstriction after drug-eluting stent implantation in pigs in vivo. Circ. J. 2015, 79, 1787.
- 97.
Nishimiya, K.; Matsumoto, Y.; Takahashi, J.; et al. Enhanced Adventitial Vasa Vasorum Formation in Patients with Vasospastic Angina: Assessment with OFDI. J. Am. Coll. Cardiol. 2016, 67, 598–600. https://doi.org/10.1016/j.jacc.2015.11.031.
- 98.
Ohyama, K.; Matsumoto, Y.; Takanami, K.; et al. Coronary Adventitial and Perivascular Adipose Tissue Inflammation in Patients with Vasospastic Angina. J. Am. Coll. Cardiol. 2018, 71, 414–425. https://doi.org/10.1016/j.jacc.2017.11.046.
- 99.
Mikami, T.; Furuhashi, M.; Numaguchi, R.; et al. Comparison of Phenotypes in Subcutaneous Fat and Perivascular Adipose Tissue Surrounding the Saphenous Vein in Coronary Artery Bypass Grafting. Circ. J. 2023, 87, 791–798. https://doi.org/10.1253/circj.CJ-22-0740.
- 100.
Mikami, T.; Dashwood, M.R.; Kawaharada, N.; et al. An Obligatory Role of Perivascular Adipose Tissue in Improved Saphenous Vein Graft Patency in Coronary Artery Bypass Grafting. Circ. J. 2024, 88, 845–852. https://doi.org/10.1253/circj.CJ-23-0581.
- 101.
Ferrari, G.; Loayza, R.; Azari, A.; et al. Superior long-term patency of no-touch vein graft compared to conventional vein grafts in over 1500 consecutive patients. J. Cardiothorac. Surg. 2024, 19, 570. https://doi.org/10.1186/s13019-024-03057-3.
- 102.
Sigdel, S.; Udoh, G.; Albalawy, R.; et al. Perivascular Adipose Tissue and Perivascular Adipose Tissue-Derived Extracellular Vesicles: New Insights in Vascular Disease. Cells 2024, 13, 1309. https://doi.org/10.3390/cells13161309.
- 103.
Rami, A.Z.A.; Hamid, A.A.; Anuar, N.N.M.; et al. Exploring the Relationship of Perivascular Adipose Tissue Inflammation and the Development of Vascular Pathologies. Mediat. Inflamm. 2022, 2022, 2734321. https://doi.org/10.1155/2022/2734321.
- 104.
Zhang, Y.Y.; Shi, Y.N.; Zhu, N.; et al. PVAT targets VSMCs to regulate vascular remodelling: Angel or demon. J. Drug Target. 2021, 29, 467–475. https://doi.org/10.1080/1061186X.2020.1859515.
- 105.
Miao, C.Y.; Li, Z.Y. The role of perivascular adipose tissue in vascular smooth muscle cell growth. Br. J. Pharmacol. 2012, 165, 643–658. https://doi.org/10.1111/j.1476-5381.2011.01404.x.
- 106.
Ford, C.A.; Mong, K.; Tabrizchi, R. Influence of tangential stress on mechanical responses to vasoactive agents in human saphenous vein with and without perivascular adipose tissue. Can. J. Cardiol. 2006, 22, 1209–1216. https://doi.org/10.1016/S0828-282X(06)70961-8.
- 107.
Ozen, G.; Topal, G.; Gomez, I.; et al. Control of human vascular tone by prostanoids derived from perivascular adipose tissue. Prostaglandins Other Lipid Mediat. 2013, 107, 13–17. https://doi.org/10.1016/j.prostaglandins.2013.06.002.
- 108.
Foudi, N.; Kotelevets, L.; Gomez, I.; et al. Differential reactivity of human mammary artery and saphenous vein to prostaglandin E2: Implication for cardiovascular grafts. Br. J. Pharmacol. 2011, 163, 826–834. https://doi.org/10.1111/j.1476-5381.2011.01264.x.
- 109.
Dashwood, M.; Souza, D.; Topal, G. Advancing coronary artery bypass grafting: The fasudil-nitroglycerin cocktail as a potential antispastic solution. J. Thorac. Dis. 2024, 16, 2694. https://doi.org/10.21037/jtd-23-1953.
- 110.
Hou, H.T.; Wang, Z.Q.; Wang, J.; et al. Antispastic Effect of Fasudil and Cocktail of Fasudil and Nitroglycerin in Internal Thoracic Artery. Ann. Thorac. Surg. 2023, 115, 1152–1161. https://doi.org/10.1016/j.athoracsur.2021.11.079.
- 111.
Chanda, J.; Brichkov, I.; Canver, C.C. Prevention of radial artery graft vasospasm after coronary bypass. Ann. Thorac. Surg. 2000, 70, 2070–2074. https://doi.org/10.1016/s0003-4975(00)02001-4.
- 112.
He, G.W.; Yang, C.Q. Use of verapamil and nitroglycerin solution in preparation of radial artery for coronary grafting. Ann. Thorac. Surg. 1996, 61, 610–614. https://doi.org/10.1016/0003-4975(95)00920-5.
- 113.
He, G.W. Verapamil plus nitroglycerin solution maximally preserves endothelial function of the radial artery: Comparison with papaverine solution. J. Thorac. Cardiovasc. Surg. 1998, 115, 1321–1327. https://doi.org/10.1016/S0022-5223(98)70215-6.
- 114.
He, G.W.; Rosenfeldt, F.L.; Buxton, B.F.; et al. Reactivity of human isolated internal mammary artery to constrictor and dilator agents. Implications for treatment of internal mammary artery spasm. Circulation 1989, 80, I141–I150.
- 115.
He, G.W.; Yang, C.Q. Comparative study on calcium channel antagonists in the human radial artery: Clinical implications. J. Thorac. Cardiovasc. Surg. 2000, 119, 94–100. https://doi.org/10.1016/s0022-5223(00)70222-4.
- 116.
Acar, C.; Jebara, V.A.; Portoghese, M.; et al. Revival of the radial artery for coronary artery bypass grafting. Ann. Thorac. Surg. 1992, 54, 652–660. https://doi.org/10.1016/0003-4975(92)91007-v.
- 117.
Jett, G.K.; Arcici, J.M., Jr.; Hatcher, C.R., Jr.; et al. Vasodilator drug effects on internal mammary artery and saphenous vein grafts. J. Am. Coll. Cardiol. 1988, 11, 1317–1324. https://doi.org/10.1016/0735-1097(88)90298-7.
- 118.
He, G.W.; Fan, L.; Furnary, A.; et al. A new antispastic solution for arterial grafting: Nicardipine and nitroglycerin cocktail in preparation of internal thoracic and radial arteries for coronary surgery. J. Thorac. Cardiovasc. Surg. 2008, 136, 673–680.e2. https://doi.org/10.1016/j.jtcvs.2007.12.019.
- 119.
Pillai, V.V.; Sreekanthan, R.; Karunakaran, J. Quantitative estimation of LIMA blood flow between extraluminal papavarine vs. extraluminal papavarine plus intraluminal vasodilator cocktail in CABG patients. Ann. Card. Anaesth. 2020, 23, 414–418. https://doi.org/10.4103/aca.ACA_164_19.
- 120.
Kamat, B.R.; Galli, S.J.; Barger, A.C.; et al. Neovascularization and coronary atherosclerotic plaque: Cinematographic localization and quantitative histologic analysis. Hum. Pathol. 1987, 18, 1036–1042. https://doi.org/10.1016/s0046-8177(87)80220-4.
- 121.
Johansson, B.L.; Souza, D.S.R.; Bodin, L.; et al. Slower progression of atherosclerosis in vein grafts harvested with ‘no touch’ technique compared with conventional harvesting technique in coronary artery bypass grafting: An angiographic and intravascular ultrasound study. Eur. J. Cardio-Thorac. Surg. 2010, 38, 414–419. https://doi.org/10.1016/j.ejcts.2010.02.007.
- 122.
Samano, N.; Geijer, H.; Bodin, L.; et al. The no-touch saphenous vein graft in elderly coronary bypass patients with multiple comorbidities is a promising conduit to substitute the left internal thoracic artery. J. Thorac. Cardiovasc. Surg. 2017, 154, 457–466.e3. https://doi.org/10.1016/j.jtcvs.2017.03.048.
- 123.
Kurazumi, H.; Suzuki, R.; Nawata, R.; et al. Impact of the no-touch harvesting technique on the vessel diameter of saphenous vein grafts for coronary artery bypass grafting. JTCVS Tech. 2022, 15, 87–94. https://doi.org/10.1016/j.xjtc.2022.07.005.
- 124.
Sugaya, A.; Uesugi, S.; Doi, M.; et al. Vasa vasorum of the no-touch saphenous vein graft observed using frequency-domain optical coherence tomography. Interdiscip. CardioVascular Thorac. Surg. 2024, 39, ivae167. https://doi.org/10.1093/icvts/ivae167.

This work is licensed under a Creative Commons Attribution 4.0 International License.