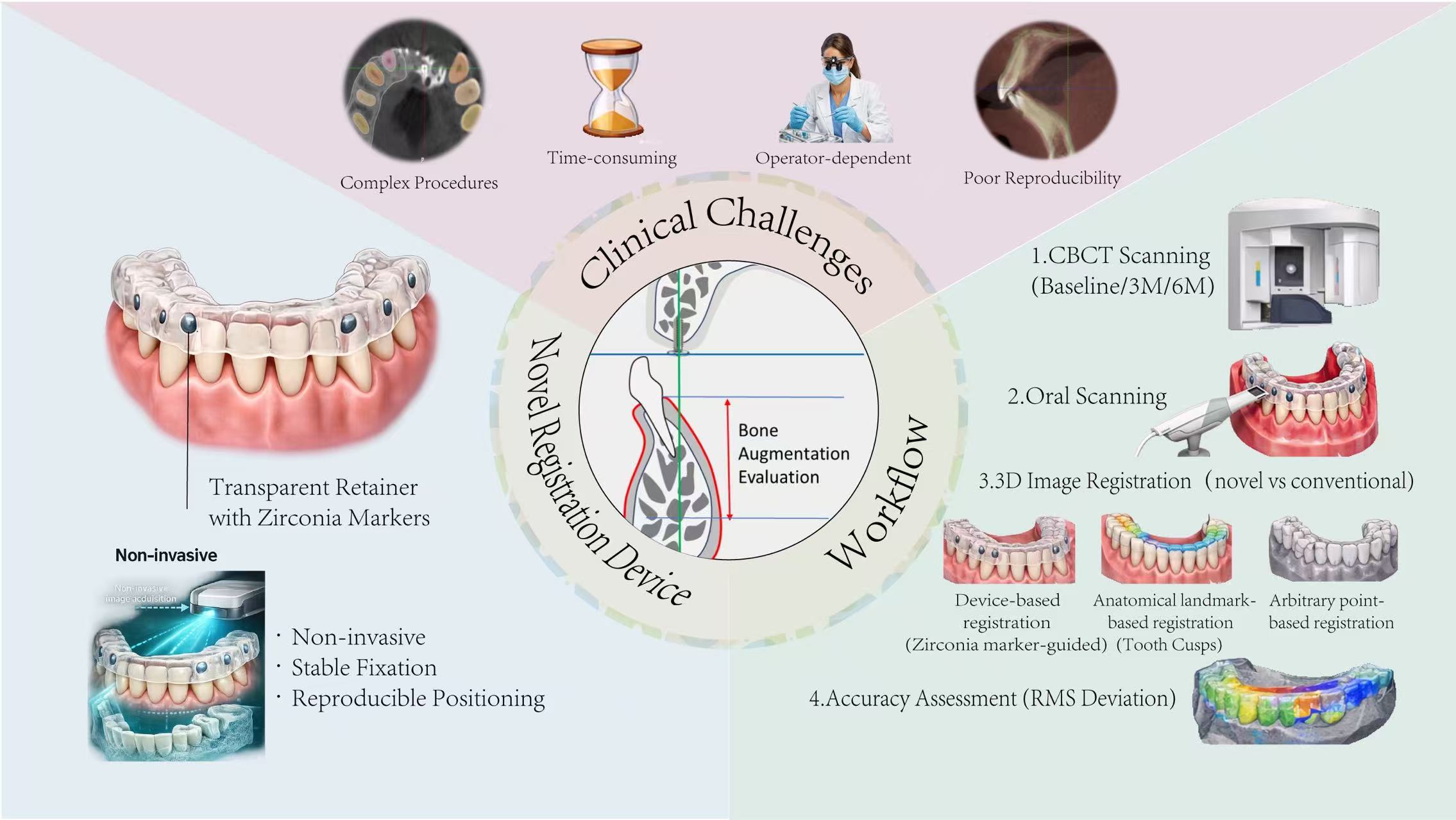
Accurate evaluation of bone augmentation is essential for surgical planning in dental implantology, and it is also crucial for validating the efficiency of bone augmentation approaches. However, the prevailing evaluation methods are complicated, time-consuming, operator-dependent, and hardly reproducible, undermining their feasibility and reliability in clinic. In response to these limitations, a registration apparatus composed of a transparent orthodontic retainer and radiographic markers was developed, enabling image superimposition before and after bone augmentation. A mandibular specimen underwent cone beam computed tomography (CBCT) scans at baseline, three, and six months, with and without the apparatus. Image registrations were independently performed by two examiners using the registration apparatus and two alternative methods. Root mean square (RMS) deviations were calculated to quantify registration accuracy. Statistical analyses were conducted using ANOVA and paired t-tests. Significant differences in RMS deviations were observed between the registration methods (p = 0.002), and using the registration apparatus achieved the lowest RMS deviation (0.055 ± 0.030 mm) and consistency at different timepoints (p = 0.856) and examiners (p = 0.441). This registration apparatus demonstrated high accuracy and reproducibility in bone augmentation evaluation, making it a potential reliable tool for quantitative evaluation of bone augmentation in dental implantology.
- Open Access
- Article
Dental Brace Register for Accurate and Reproducible Bone Augmentation Evaluation in Dental Implantology
- Zhifan Sun 1,2,3,†,
- Jiayuan Zhang 4,†,
- Xuemei Xie 5,
- Lingfei Wei 6,
- Chunfeng Xu 1,2,3,7,*,
- Dedong Yu 1,2,3,5,*
Author Information
Received: 07 Mar 2026 | Revised: 31 Mar 2026 | Accepted: 01 Apr 2026 | Published: 13 Apr 2026
Abstract
Graphical Abstract
Keywords
bone augmentation evaluation | accuracy and reproducibility | three-dimensional image registration | dental implantology
References
- 1.
Gargallo-Albiol, J. How to Enhance Dental Implant Therapies and Definitive Restoration Outcomes to Reduce Complications and Improve Patient Well-Being. Materials 2023, 16, 3730.
- 2.
Bassir, S.H.; Alhareky, M.; Wangsrimongkol, B.; et al. Systematic Review and Meta-Analysis of Hard Tissue Outcomes of Alveolar Ridge Preservation. Int. J. Oral. Maxillofac. Implants 2018, 33, 979–994.
- 3.
Stumbras, A.; Kuliesius, P.; Januzis, G.; et al. Alveolar Ridge Preservation after Tooth Extraction Using Different Bone Graft Materials and Autologous Platelet Concentrates: A Systematic Review. J. Oral. Maxillofac. Res. 2019, 10, e2.
- 4.
Tan, W.L.; Wong, T.L.; Wong, M.C.; et al. A systematic review of post-extractional alveolar hard and soft tissue dimensional changes in humans. Clin. Oral. Implants Res. 2012, 23, 1–21.
- 5.
MacBeth, N.; Trullenque-Eriksson, A.; Donos, N.; et al. Hard and soft tissue changes following alveolar ridge preservation: A systematic review. Clin. Oral. Implants Res. 2017, 28, 982–1004.
- 6.
D’haese, J.; Ackhurst, J.; Wismeijer, D.; et al. Current state of the art of computer-guided implant surgery. Periodontol. 2000 2017, 73, 121–133.
- 7.
Sethi, A.; Kaus, T.; Sharma, N. Clinical record-keeping for monitoring treatment outcomes in implant dentistry: A case study. Prim. Dent. J. 2013, 2, 39–43.
- 8.
MacBeth, N.D.; Donos, N.; Mardas, N. Alveolar ridge preservation with guided bone regeneration or socket seal technique. A randomised, single-blind controlled clinical trial. Clin. Oral. Implants Res. 2022, 33, 681–699.
- 9.
Lutz, R.; Neukam, F.W.; Simion, M.; et al. Long-term outcomes of bone augmentation on soft and hard-tissue stability: A systematic review. Clin. Oral. Implants Res. 2015, 26, 103–122.
- 10.
El-Gamal, F.E.Z.A.; Elmogy, M.; Atwa, A. Current trends in medical image registration and fusion. Egyptian Informatics Journal 2016, 17, 99–124.
- 11.
Park, J.H.; Hwang, C.J.; Choi, Y.J.; et al. Registration of digital dental models and cone-beam computed tomography images using 3-dimensional planning software: Comparison of the accuracy according to scanning methods and software. Am. J. Orthod. Dentofacial Orthop. 2020, 157, 843–851.
- 12.
Flügge, T.; Derksen, W.; Te Poel, J.; et al. Registration of cone beam computed tomography data and intraoral surface scans—A prerequisite for guided implant surgery with CAD/CAM drilling guides. Clin. Oral. Implants Res. 2017, 28, 1113–1118.
- 13.
Zou, J.; Gao, B.; Song, Y.; et al. A review of deep-based deformable medical image registration. Front. Oncol. 2022, 12, 1047215.
- 14.
Yang, S.; Dong, B.; Zhang, Q.; et al. An Indirect Digital Technique to Transfer 3D Printed Casts to a Mechanical Articulator with Individual Sagittal Condylar Inclination Settings Using CBCT and Intraoral Scans. J. Prosthodont. 2022, 31, 822–827.
- 15.
Porter, B.C.; Rubens, D.J.; Strang, J.G.; et al. Three-dimensional registration and fusion of ultrasound and MRI using major vessels as fiducial markers. IEEE Trans. Med. Imaging 2001, 20, 354–359.
- 16.
Lan, K.; Tao, B.; Wang, F.; et al. Accuracy evaluation of 3D-printed noninvasive adhesive marker for dynamic navigation implant surgery in a maxillary edentulous model: An in vitro study. Med. Eng. Phys. 2022, 103, 103783.
- 17.
Wang, J.; Shen, Y.; Yang, S. A practical marker-less image registration method for augmented reality oral and maxillofacial surgery. Int. J. Comput. Assist. Radiol. Surg. 2019, 14, 763–773.
- 18.
Lee, W.; Lee, S.; Chong, S.; et al. Radiation dose reduction and improvement of image quality in digital chest radiography by new spatial noise reduction algorithm. PLoS ONE 2020, 15, e0228609.
- 19.
Naik, R.R.; Hoblidar, A.; Bhat, S.N.; et al. A Hybrid 3D-2D Image Registration Framework for Pedicle Screw Trajectory Registration between Intraoperative X-ray Image and Preoperative CT Image. J. Imaging 2022, 8, 185.
- 20.
Fang, S.B.; Yang, G.J.; Kang, Y.F.; et al. Method and accuracy of determining the jaw position of repositioning splint with the aid of digital technique. Beijing Da Xue Xue Bao Yi Xue Ban 2020, 53, 76–82.
- 21.
Swennen, G.R.; Barth, E.L.; Eulzer, C.; et al. The use of a new 3D splint and double CT scan procedure to obtain an accurate anatomic virtual augmented model of the skull. Int. J. Oral. Maxillofac. Surg. 2007, 36, 146–152.
- 22.
Zheng, R.; Ye, J.; Zhang, X.; et al. Influence factors on registration of three-dimensional contrast-enhanced ultrasound fusion imaging in evaluating the ablative margin—A phantom study. Clin. Hemorheol. Microcirc. 2023, 83, 117–128.
- 23.
Blokker, A.M.; Wood, R.; Milner, J.C.; et al. Novel quantification of the regional strain distribution in the anterior cruciate ligament in response to simulated loading using micro-CT imaging. J. Exp. Orthop. 2021, 8, 95.
- 24.
Ketcha, M.D.; de Silva, T.; Han, R.; et al. Fundamental limits of image registration performance: Effects of image noise and resolution in CT-guided interventions. Proc. SPIE Int. Soc. Opt. Eng. 2017, 10135, 62–69.
- 25.
Luu, H.M.; Klink, C.; Niessen, W.; et al. Non-Rigid Registration of Liver CT Images for CT-Guided Ablation of Liver Tumors. PLoS ONE 2016, 11, e0161600.
- 26.
Kim, C.; et al. An additional tilted-scan-based CT metal-artifact-reduction method for radiation therapy planning. J. Appl. Clin. Med. Phys. 2019, 20, 237–249.
- 27.
Brock, K.K.; Mutic, S.; McNutt, T.R.; et al. Use of image registration and fusion algorithms and techniques in radiotherapy: Report of the AAPM Radiation Therapy Committee Task Group No. 132. Med. Phys. 2017, 44, e43–e76.
- 28.
Gooding, M.J.; Eccles, C.L.; Fuss, M.; et al. Assessing The Quality of Deformable CT-MR Registration for the Purpose of Multimodal Radiotherapy Contouring. Int. J. Radiat. Oncol. Biol. Phys. 2011, 81, S812–S813.
- 29.
Swennen, G.R.; Mommaerts, M.Y.; Abeloos, J.; et al. A cone-beam CT based technique to augment the 3D virtual skull model with a detailed dental surface. Int. J. Oral. Maxillofac. Surg. 2009, 38, 48–57.
- 30.
Berry, J.; O’Malley, B.W, Jr.; Humphries, S.; et al. Making image guidance work: Understanding control of accuracy. Ann. Otol. Rhinol. Laryngol. 2003, 112, 689–692.
- 31.
Schaefer, O.; Watts, D.C.; Sigusch, B.W.; et al. Marginal and internal fit of pressed lithium disilicate partial crowns in vitro: A three-dimensional analysis of accuracy and reproducibility. Dent. Mater. 2012, 28, 320–326.
- 32.
Elhawary, H.; Oguro, S.; Tuncali, K.; et al. Multimodality non-rigid image registration for planning, targeting and monitoring during CT-guided percutaneous liver tumor cryoablation. Acad. Radiol. 2010, 17, 1334–1344.
- 33.
Mehl, A.; Reich, S.; Beuer, F.; et al. Accuracy, trueness, and precision—A guideline for the evaluation of these basic values in digital dentistry. Int. J. Comput. Dent. 2021, 24, 341–352.

This work is licensed under a Creative Commons Attribution 4.0 International License.


