Previous studies showed an increased risk of COVID-19 in several occupations, particularly healthcare workers. We aimed to explore whether night shift work, a possible determinant of immune suppression, might have contributed to COVID infection in the pre-vaccine months using data from 435 Italian participants (330 women, 105 men) to the COVISTRESS online survey. After adjusting for age, sex, and education, the risk of COVID-19 was elevated among night shift workers (OR = 5.5, 95% CI 2.92, 10.2), particularly among healthcare workers (OR = 8.7, 95% CI 4.07, 18.4). After excluding healthcare workers from the analysis, subjects working night shifts in other jobs also run a 5-fold elevated risk of COVID-19 (OR = 5.1, 95% CI 1.92, 18.4), which was confirmed in a sensitivity analysis excluding subjects who reported working remotely. Parenting school-aged children was also a significant predictor (OR = 2.5; 95% CI 1.20–5.21) of SARS-CoV-2 infection, but there was no interaction with night shift work. Education, marital status, smoking, and sleep quality did not account for the association with night shift work. Our results suggest that, during the 2020 COVID-19 pandemic, night shift workers run an excess risk of COVID-19 infection. Whether this was because of sleep loss-induced suppression of the immune system, confounding, or chance remains to be clarified.
- Open Access
- Article
Covid-19 and Shift Work: A Preliminary Note from the COVISTRESS Online Survey
- Monica Puligheddu 1,*,†,
- Elvia Battaglia 2,†,
- Rosamaria Lecca 1,
- Elisa Casaglia 1,
- Michela Figorilli 1,
- Valerio Cancedda 3,
- Sara De Matteis 4,
- Maëlys Clinchamps 5,
- Reza Bagheri 6,
- Morteza Charkhabi 7,
- Maria Livia Fantini 5,
- on behalf of the COVISTRESS Network ‡,
- Frederic Dutheil 5
Author Information
Received: 11 Jan 2026 | Revised: 19 Mar 2026 | Accepted: 24 Mar 2026 | Published: 15 Apr 2026
Abstract
Graphical Abstract
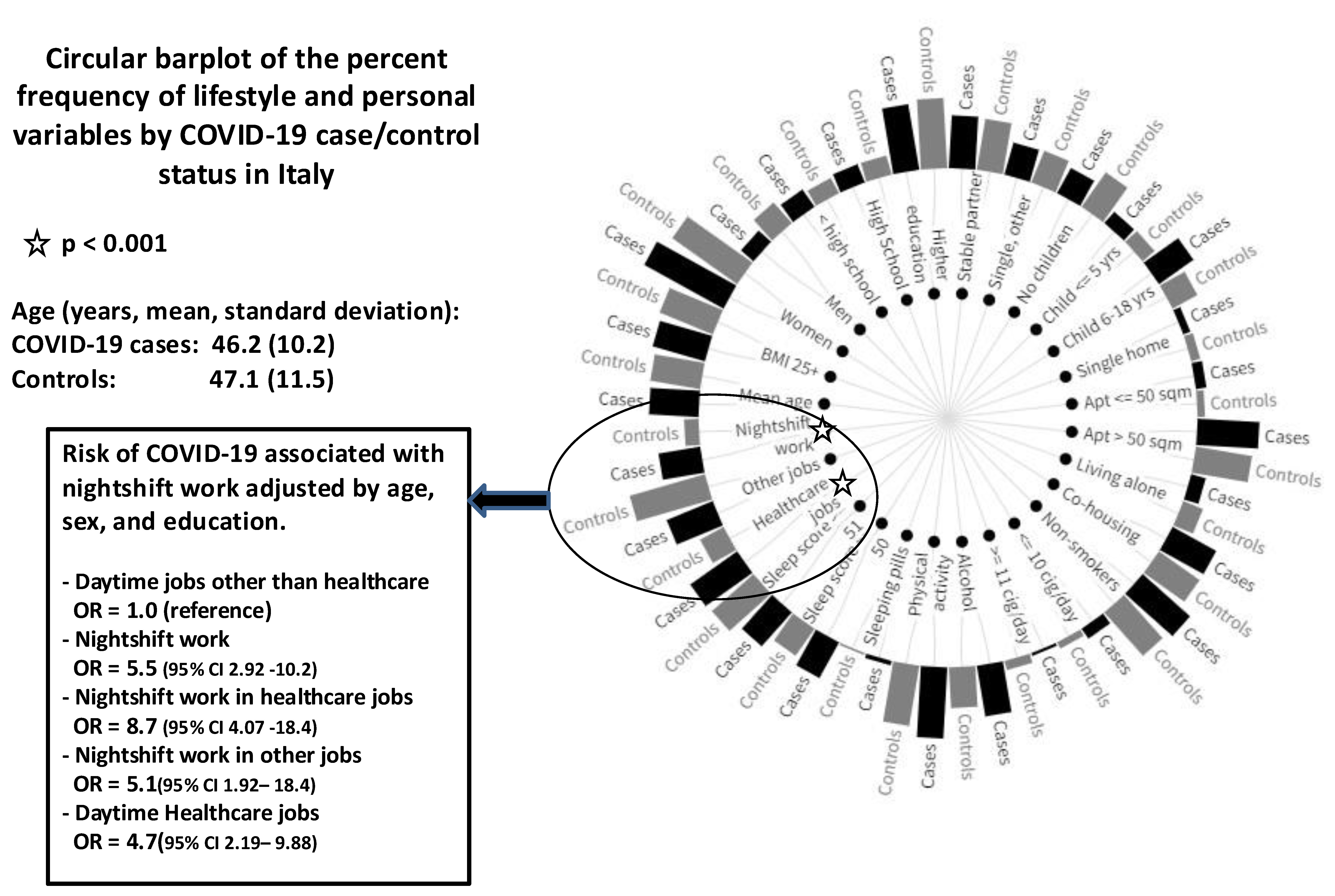
Keywords
COVID-19 | occupational exposure | shift work | sleep wake disorders | immunologic factors
References
- 1.
Lan, F.Y.; Wei, C.F.; Hsu, Y.T.; et al. Work-related COVID-19 transmission in six Asian countries/areas: A follow-up study. PLoS ONE 2020, 15, e0233588.
- 2.
Mutambudzi, M.; Niedwiedz, C.; Macdonald, E.B.; et al. Occupation and risk of severe COVID-19: Prospective cohort study of 120 075 UK Biobank participants. Occup. Env. Environ. Med. 2020, 78, 307–314.
- 3.
Agius, R.M. Covid-19: Statutory means of scrutinizing workers’ deaths and disease. Occup. Med. 2020, 70, 515–522.
- 4.
Thorkildsen, M.S.; Gusad, L.T.; Damås, J.K. The Effects of Shift Work on the Immune System: A Narrative Review. Sleep Sci. 2023, 16, e368–e374.
- 5.
Irwin, M. Effects of sleep and sleep loss on immunity and cytokines. Brain Behav. Immun. 2002, 16, 503–512.
- 6.
Nukiwa, R.; Oda, S.; Matsumoto, H.; et al. Changes in gene expression in healthcare workers during night shifts: Implications for immune response and health risks. J. Int. Care 2025, 13, 14.
- 7.
Silva, F.R.; Guerreiro, R.C.; Andrade, H.A.; et al. Does the compromised sleep and circadian disruption of night and shiftworkers make them highly vulnerable to 2019 coronavirus disease (COVID-19)? Chronobiol. Int. 2020, 37, 607–617.
- 8.
Loef, B.; Bosma, E.; van Kerkhof, L.W.M.; et al. Night-shift work and susceptibility to infectious diseases: A systematic review and meta-analysis. Scand. J. Work. Env. Environ. Health 2025, 51, 298–311.
- 9.
Fatima, Y.; Bucks, R.S.; Mamun, A.A.; et al. Shift work is associated with increased risk of COVID-19: Findings from the UK Biobank cohort. J. Sleep. Res. 2021, 30, e13326.
- 10.
Maidstone, R.; Anderson, S.G.; Ray, D.W.; et al. Shift work is associated with positive COVID-19 status in hospitalised patients. Thorax 2021, 76, 601–606.
- 11.
Ugbolue, U.C.; Duclos, M.; Urzeala, C.; et al. An Assessment of the Novel COVISTRESS Questionnaire: COVID-19 Impact on Physical Activity, Sedentary Action and Psychological Emotion. J. Clin. Med. 2020, 9, 3352.
- 12.
ILOSTAT. International Standards Classification of Occupations (ISCO). Available online: https://ilostat.ilo.org/methods/concepts-and-definitions/classification-occupation/ (accessed on 28 December 2023).
- 13.
Wang, X.; Jiang, X.; Huang, Q.; et al. Risk factors of SARS-CoV-2 infection in healthcare workers: A retrospective study of a nosocomial outbreak. Sleep Med. X 2020, 2, 100028.
- 14.
Martin, C.A.; Pan, D.; Melbourne, C.; et al. Risk factors associated with SARS-CoV-2 infection in a multiethnic cohort of United Kingdom healthcare workers (UK-REACH): A cross-sectional analysis. PLoS Med. 2022, 19, e1004015.
- 15.
Bollinger, T.; Bollinger, A.; Oster, H.; et al. Sleep, immunity, and circadian clocks: A mechanistic model. Gerontology 2010, 56, 574–580.
- 16.
Prather, A.A.; Leung, C.W. Association of insufficient sleep with respiratory infection among adults in the United States. JAMA Intern. Med. 2016, 176, 850–852.
- 17.
Besedovsky, L.; Lange, T.; Haack, M. The sleep-immune crosstalk in health and disease. Physiol. Rev. 2019, 99, 1325–1380.

This work is licensed under a Creative Commons Attribution 4.0 International License.


