Background: Brexpiprazole, a third-generation antipsychotic with partial dopamine D2/D3 and serotonin 5-HT1A agonist properties, has emerged as a promising therapeutic option for patients with schizophrenia, including those with comorbid substance use disorders (SUDs). Managing psychosis in the presence of substance use represents a major clinical challenge, often associated with poorer outcomes, reduced adherence, and increased relapse risk. Methods: This narrative review(non-systematic) synthesizes evidence from randomized controlled trials, observational real-world studies, and expert consensus reports published between 2020 and 2026. The literature was examined to evaluate the pharmacological mechanisms, clinical efficacy, safety, and practical use of brexpiprazole in psychotic disorders, with particular attention to populations with comorbid substance use disorders. As a narrative review, this work does not employ systematic search protocols or quality appraisal tools; findings should be interpreted with this methodological limitation in mind. Results: Available evidence suggests that brexpiprazole can meaningfully reduce both positive and negative symptoms of psychosis, while also demonstrating beneficial effects on substance craving and functional outcomes in patients with dual diagnoses. Across randomized and real-world studies, brexpiprazole shows a favorable tolerability profile, characterized by minimal activation, low sedation, reduced risk of extrapyramidal symptoms, and limited cardiometabolic burden. These properties support its use in complex clinical populations requiring long-term treatment and polypharmacological management. Clinical Implications and Decision-Making: Based on the available evidence, brexpiprazole may be particularly suitable for: (1) patients with prominent negative symptoms requiring improvement in motivation and social functioning; (2) individuals with comorbid substance use disorders, particularly stimulant use, where dopaminergic modulation may address both psychotic symptoms and craving; (3) patients who have experienced significant metabolic or motor side effects with other antipsychotics; (4) individuals requiring cognitive preservation or enhancement. However, clinicians should consider that most evidence derives from relatively short-term studies with selected populations, and long-term real-world effectiveness data remain limited. Treatment decisions should be individualized based on symptom profile, comorbidity burden, prior medication responses, and patient preferences. Conclusions: Brexpiprazole represents a clinically valuable option for the management of psychosis, particularly in patients with comorbid substance use disorders. Its balanced pharmacological profile, combined with consistent efficacy and good tolerability, supports its role in integrated, long-term treatment strategies for complex and dual-diagnosis populations.
- Open Access
- Review
Brexpiprazole in the Management of Schizophrenia and Comorbid Substance Use Disorders: A Narrative Review of Efficacy, Safety, and Real-World Evidence (2020–2026)
- Miriam Olivola 1,2,3,*,
- Nicolaja Girone 2,3,
- Andrea Crippa 2,3,
- Monica Macellaro 2,3,
- Vassilis Martiadis 4,
- Fabiola Raffone 4,
- Tiziano Prodi 2,3,
- Natascia Brondino 1,
- Roberta Anniverno 2,
- Bernardo Dell’Osso 2,3,5,6
Author Information
Received: 09 Jan 2026 | Revised: 27 Jan 2026 | Accepted: 11 Feb 2026 | Published: 26 Feb 2026
Abstract
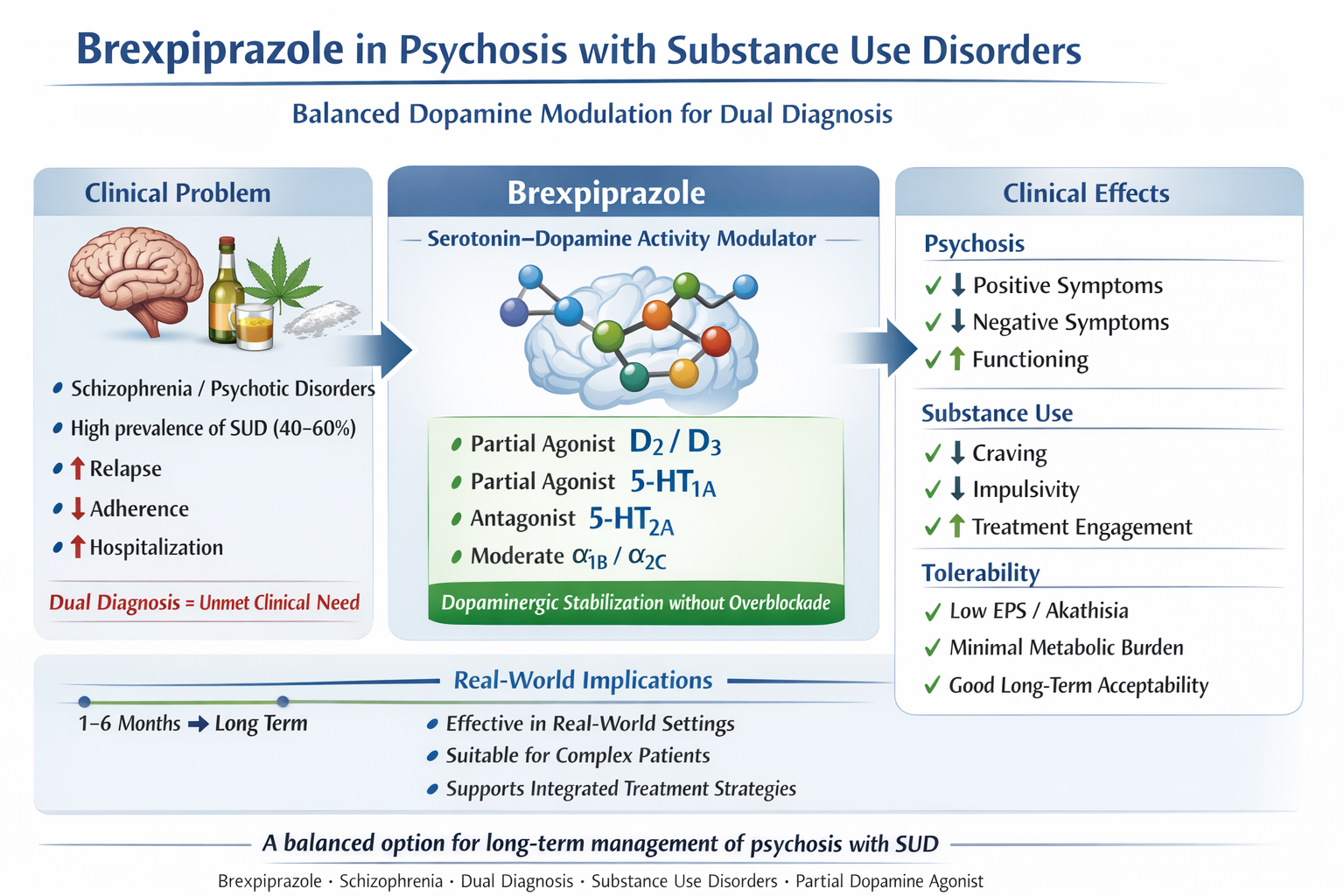
Graphical Abstract
Keywords
brexpiprazole | schizophrenia | substance use disorders | dual diagnosis | partial dopamine agonists | antipsychotic pharmacology
References
- 1.
Fan, X.; Freudenreich, O.; Jarskog, L.F.; et al. Brexpiprazole for the Treatment of Co-occurring Schizophrenia and Substance Use Disorder: A Multisite, Randomized, Controlled Trial. J. Clin. Psychiatry 2025, 86, 25m15786. https://doi.org/10.4088/JCP.25m15786.
- 2.
Correll, C.U.; Mafi, C.E.; Fagiolini, A.; et al. Brexpiprazole in the Management of Schizophrenia: A Consensus Report of Best Practices from Acute to Maintenance Treatment. Neuropsychiatr. Dis. Treat. 2025, 21, 1857–1883. https://doi.org/10.2147/NDT.S539306.
- 3.
Neyra, A.; Parro-Torres, C.; Ros-Cucurull, E.; et al. Management of Schizophrenia and Comorbid Substance Use Disorders: Expert Review and Guidance. Ann. Gen. Psychiatry 2024, 23, 40. https://doi.org/10.1186/s12991-024-00529-7.
- 4.
Chiappini, S.; Cavallotto, C.; Mosca, A.; et al. Investigating the Effectiveness of Brexpiprazole in Schizophrenic Patients with Concurrent Alcohol and Substance Use Disorder: A Prospective, Multicentric, Real-World Study. Preprints 2024, 17, 535. https://doi.org/10.20944/preprints202401.1404.v1.
- 5.
Ricci, V.; Sarni, A.; Martinotti, G.; et al. Comparative Analysis of Third-Generation Antipsychotics in First-Episode Schizophrenia: Efficacy, Safety, and Cognitive Impacts. A Narrative Review. Int. Clin. Psychopharmacol. 2024, 40, 191–206. https://doi.org/10.1097/yic.0000000000000559.
- 6.
Bogusz, K.; Wojnar, M. Brexpiprazole in the Treatment of Schizophrenia: Pharmacology, Efficacy, and Side Effects Profile. Pharmacother. Psychiatry Neurol. 2022, 38, 107–118. https://doi.org/10.5114/fpn.2022.124607.
- 7.
Hishimoto, A.; Yasui-Furukori, N.; Sekine, D.; et al. Treatment Discontinuation Among Patients with Schizophrenia Treated with Brexpiprazole and Other Oral Atypical Antipsychotics in Japan: A Retrospective Observational Study. Adv. Ther. 2022, 39, 4299–4314. https://doi.org/10.1007/s12325-022-02252-9.
- 8.
Leucht, S.; Cipriani, A.; Spineli, L.; et al. Comparative Efficacy and Tolerability of 15 Antipsychotic Drugs in Schizophrenia: A Multiple-Treatments Meta-Analysis. Lancet 2013, 382, 951–962. https://doi.org/10.1016/S0140-6736(13)60733-3.
- 9.
Fusar-Poli, P.; Papanastasiou, E.; Stahl, D.; et al. Treatments of Negative Symptoms in Schizophrenia: Meta-Analysis of 168 Randomized Placebo-Controlled Trials. Schizophr. Bull. 2015, 41, 892–899. https://doi.org/10.1093/schbul/sbu170.
- 10.
Velligan, D.I.; Weiden, P.J.; Sajatovic, M.; et al. The Expert Consensus Guideline Series: Adherence Problems in Patients with Serious and Persistent Mental Illness. J. Clin. Psychiatry 2009, 70, 1–48.
- 11.
Correll, C.U.; Robinson, D.G.; Schooler, N.R.; et al. Cardiometabolic Risk in Patients with First-Episode Schizophrenia Spectrum Disorders: Baseline Results from the RAISE-ETP Study. JAMA Psychiatry 2014, 71, 1350–1363. https://doi.org/10.1001/jamapsychiatry.2014.1314.
- 12.
Watanabe, Y.; Yamada, S.; Otsubo, T.; et al. Brexpiprazole for the Treatment of Schizophrenia in Adults: An Overview of Its Clinical Efficacy and Safety and a Psychiatrist’s Perspective. Drug Des. Dev. Ther. 2020, 14, 1559–1577. https://doi.org/10.2147/DDDT.S240859.
- 13.
Edinoff, A.N.; Wu, N.W.; Maxey, B.S.; et al. Brexpiprazole for the Treatment of Schizophrenia and Major Depressive Disorder: A Comprehensive Review of Pharmacological Considerations in Clinical Practice. Psychopharmacol. Bull. 2021, 51, 69–95.
- 14.
Siwek, M.; Wojtasik-Bakalarz, K.; Krupa, A.J.; et al. Brexpiprazole—Pharmacologic Properties and Use in Schizophrenia and Mood Disorders. Brain Sci. 2023, 13, 397. https://doi.org/10.3390/brainsci13030397.
- 15.
Bieńkowski, P.; Wichniak, A. Efficacy and Tolerability of Brexpiprazole—A New Antipsychotic Drug from the Group of Dopamine D2 Receptor Partial Agonists. Psychiatr. Pol. 2024, 58, 237–248. https://doi.org/10.12740/pp/onlinefirst/169646.
- 16.
Kishi, T.; Ikuta, T.; Matsuda, Y.; et al. Aripiprazole vs. Brexpiprazole for Acute Schizophrenia: A Systematic Review and Network Meta-Analysis. Psychopharmacology 2020, 237, 1459–1470. https://doi.org/10.1007/S00213-020-05472-5.
- 17.
Trovini, G.; Lombardozzi, G.; Kotzalidis, G.D.; et al. Partial Dopamine D2/3 Agonists and Dual Disorders: A Retrospective-Cohort Study in a Real-World Clinical Setting on Patients with Schizophrenia Spectrum Disorders and Cannabis Use Disorder. Curr. Neuropharmacol. 2025, 23, 996–1006. https://doi.org/10.2174/011570159x350599241214042724.
- 18.
Lombardozzi, G.; Trovini, G.; Amici, E.; et al. Brexpiprazole in Patients with Schizophrenia with or Without Substance Use Disorder: An Observational Study. Front. Psychiatry 2023, 14, 1321233. https://doi.org/10.3389/fpsyt.2023.1321233.
- 19.
Zhao, M.; Qin, B.; Mao, Y.; et al. Efficacy and Safety of Low-Dose Brexpiprazole for Acute Schizophrenia: Meta-Analysis of Randomized Placebo-Controlled Trials. Neuropsychiatr. Dis. Treat. 2022, 18, 1989–2000. https://doi.org/10.2147/NDT.S374577.
- 20.
Correll, C.; Pflug, B.; Zhang, Z.; et al. Efficacy and Safety of Brexpiprazole in Early-Episode Schizophrenia: Post Hoc Analysis of Clinical Trials in Adults and Adolescents. Eur. Psychiatry 2025, 68, S1093. https://doi.org/10.1192/j.eurpsy.2025.2211.
- 21.
Patel, M.X.; Nikolaou, V.; David, A.S. Psychiatrists’ Attitudes to Maintenance Medication for Patients with Schizophrenia. Psychol. Med. 2003, 33, 83–89.
- 22.
Jin, H.; Shih, G.; Golshan, S.; et al. Comparison of Longer-Term Safety and Effectiveness of 4 Atypical Antipsychotics in Patients over Age 40: A Trial Using Equipoise-Stratified Randomization. J. Clin. Psychiatry 2013, 74, 10–18. https://doi.org/10.4088/JCP.12m08001.
- 23.
Inada, K.; Yamada, S.; Akiyoshi, H.; et al. Long-Term Efficacy and Safety of Brexpiprazole in Elderly Japanese Patients with Schizophrenia: A Subgroup Analysis of an Open-Label Study. Neuropsychiatr. Dis. Treat. 2020, 16, 2789–2803. https://doi.org/10.2147/NDT.S265173.
- 24.
Brasso, C.; Colli, G.; Sgro, R.; et al. Efficacy of Serotonin and Dopamine Activity Modulators in the Treatment of Negative Symptoms in Schizophrenia: A Rapid Review. Biomedicines 2023, 11, 921. https://doi.org/10.3390/biomedicines11030921.
- 25.
Ricci, V.; Paggi, A.; Cristofori, E.; et al. Efficacy of Brexpiprazole for Treatment Persistent Negative Symptoms in Three Schizophrenic Patients: A Case Series. Psychiatry Res. Case Rep. 2022, 1, 100040. https://doi.org/10.1016/j.psycr.2022.100040.
- 26.
Chiappini, S.; Cavallotto, C.; Mosca, A.; et al. Investigating the Effectiveness of Brexpiprazole in Subjects with Schizophrenia Spectrum Illness and Co-Occurring Substance Use Disorder: A Prospective, Multicentric, Real-World Study. Pharmaceuticals 2024, 17, 535. https://doi.org/10.3390/ph17040535.
- 27.
Murrie, B.; Lappin, J.; Large, M.; et al. Transition of Substance-Induced, Brief, and Atypical Psychoses to Schizophrenia: A Systematic Review and Meta-Analysis. Schizophr. Bull. 2020, 46, 505–516. https://doi.org/10.1093/schbul/sbz102.
- 28.
Kendler, K.S.; Gallagher, T.J.; Abelson, J.M.; et al. Lifetime Prevalence, Demographic Risk Factors, and Diagnostic Validity of Nonaffective Psychosis as Assessed in a US Community Sample. Arch. Gen. Psychiatry 1996, 53, 1022–1031.
- 29.
Stroup, T.S.; Gray, N. Management of Common Adverse Effects of Antipsychotic Medications. World Psychiatry 2018, 17, 341–356. https://doi.org/10.1002/wps.20567.
- 30.
Di Nicola, M.; Pepe, M.; Milintenda, M.; et al. Patient Life Engagement and Metabolic Profile Improve After Switching from First-/Second-Generation Antipsychotics to Brexpiprazole: A Real-World Study in Patients with Schizophrenia. J. Pers. Med. 2025, 15, 502. https://doi.org/10.3390/jpm15110502.
- 31.
Ward, C.; Milovančević, M.P.; Kohegyi, E.; et al. Efficacy and Safety of Brexpiprazole in Adolescents with Schizophrenia: A Multicountry, Randomised, Double-Blind, Placebo-Controlled, Phase 3 Trial with an Active Reference. Lancet Psychiatry 2025, 12, 345–354. https://doi.org/10.1016/S2215-0366(25)00043-4.
- 32.
Crump, C.J.; Abuelazm, H.; Ibrahim, K.; et al. An Overview of the Efficacy and Safety of Brexpiprazole for the Treatment of Schizophrenia in Adolescents. Expert Rev. Neurother. 2024, 24, 727–733. https://doi.org/10.1080/14737175.2024.2367695.
- 33.
Meade, N.; Shi, L.; Meehan, S.R.; et al. Efficacy and Safety of Brexpiprazole in Patients with Schizophrenia Presenting with Severe Symptoms: Post-Hoc Analysis of Short- and Long-Term Studies. J. Psychopharmacol. 2020, 34, 829–838. https://doi.org/10.1177/0269881120936485.
- 34.
Phalguni, A.; McCool, R.; Wood, H.; et al. Systematic Literature Review and Network Meta-Analysis of Lurasidone, Brexpiprazole and Cariprazine for Schizophrenia. Int. Clin. Psychopharmacol. 2023, 38, 45–56. https://doi.org/10.1097/yic.0000000000000427.

This work is licensed under a Creative Commons Attribution 4.0 International License.


